Symptoms & Diagnosis
You have your annual physicals. You see your dentist regularly. You’ve got this healthcare thing down. But is your eye doctor on that list?
Regular exams keep your vision strong, but they also detect eye diseases early — many of which go unnoticed for a long time.
During an eye exam, an optometrist or ophthalmologist (eye doctor) will check your:
- Visual acuity: how clearly you can see
- Eye alignment: where each eye is looking when you focus on one spot
- Eye movement: how your muscles move your eyes around
They’ll also look inside your eyes to check for signs of eye disease, such as cataracts and glaucoma, or other health problems, including high blood pressure and diabetes.
Whether your eye exam serves to help you see more clearly or to monitor your risk for eye diseases, it’s difficult to argue the benefit of getting your eyes checked.
Depending on your age, health history and even gender, recommendations for how often you should see your doctor may differ.
ReSTORA CARE uses a wide variety of tests and procedures to examine your eyes.
These tests range from simple ones, like having you identify letters on an eye chart, to complex tests, such as using digital imaging devices to see and evaluate tiny blood vessels and other structures inside your eyes.
A comprehensive eye exam can take an hour or more, depending on the doctor and the number and complexity of tests required to fully evaluate your vision and the health of your eyes.
Here are eye and vision tests that you may encounter during a comprehensive eye exam:
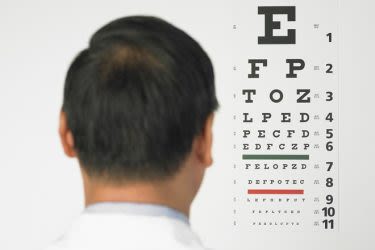
Visual acuity tests
Among the first tests performed in a comprehensive eye exam are visual acuity tests that measure the sharpness of your eyesight.
These usually are performed using a projected eye chart to measure your distance visual acuity and a small, hand-held acuity chart to measure your visual acuity at a normal reading distance.
Color blindness test
A screening test that checks your color vision often is performed early in a comprehensive eye exam to rule out color blindness.
In addition to detecting hereditary color vision deficiencies, color blind tests also can alert your eye doctor to possible eye health problems that may affect your color vision.

Cover test
While there are many ways for your eye doctor to check how your eyes work together, the cover test is the simplest and most common.
During a cover test, your eye doctor will ask you to focus on a small object across the room and will then cover each of your eyes alternately while you stare at the target. The test is then repeated with you looking at a near object.
During these tests, your eye doctor will assess whether the uncovered eye must move to pick up the fixation target, which could indicate strabismus or a more subtle binocular vision problem that could cause eye strain or amblyopia (“lazy eye”).
Ocular motility (eye movements) testing
Ocular motility testing is performed to determine how well your eyes can follow a moving object and/or quickly move between and accurately fixate on two separate targets.
To test smooth eye movements (“pursuits”), your eye doctor will have you hold your head still and ask you to follow the slow movement of a hand-held light or other target with just your eyes.
To evaluate quick eye movements (“saccades”), your doctor might have you move your eyes back and forth between two targets positioned some distance apart from each other.
Problems with eye movements can cause eye strain, headaches, blurry vision and other problems.
Stereopsis (depth perception) test
Stereopsis is the term used to describe eye teaming that enables normal depth perception and appreciation of the 3-dimensional nature of objects.
In one commonly used stereopsis test, you wear a pair of “3D” glasses and look at a booklet of test patterns. Each pattern has four small circles, and your task is to point out which circle in each pattern looks closer to you than the other three circles.
If you can correctly identify the “closer” circle in each pattern, you likely have excellent eye teaming skills that should enable you to experience normal depth perception.
Retinoscopy
In this test, your eye doctor will sit about arm’s length from you with the room lights dimmed and shine a bright light into your eyes with a hand-held instrument. This procedure can tell your doctor if you have a cataract or a significant distortion of the shape of your cornea (keratoconus).
Retinoscopy also can be used to give your doctor an approximation of your eyeglass prescription by seeing how the light reflections change as different powered lenses are placed in front of your eyes.
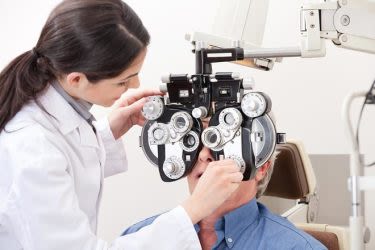
Refraction
This is the test that your eye doctor uses to determine your eyeglass prescription.
During a manual refraction, your doctor puts an instrument called a phoropter in front of your eyes and shows you a series of lens choices. He or she will then ask you which of the two lenses in each choice looks clearer.
Based on your answers, the best lens power will be fine-tuned until the eyeglass prescription that gives you the clearest vision is determined.
The refraction also determines how much nearsightedness, farsightedness or astigmatism you have.
Autorefractors and aberrometers
Your eye doctor also may use an autorefractor or aberrometer to automatically estimate your eyeglass prescription. With both devices, a chin rest stabilizes your head while you look into the instrument at a pinpoint of light or a detailed image.
An autorefractor, like a manual refraction, determines the lens power required to accurately focus light on your retina. Autorefractors are especially helpful for determining an eyeglass prescription for young children and other patients who may have trouble sitting still, paying attention and providing feedback that the eye doctor needs to perform an accurate manual refraction.
Studies have shown that modern autorefractors are very accurate. They also save time. The autorefraction takes only a few seconds, and the results obtained from the automated test greatly reduce the time required for your eye doctor to perform a manual refraction and determine your eyeglass prescription.
An aberrometer uses advanced wavefront technology to detect even obscure vision errors based on the way light travels through your eye.
Aberrometers primarily are used for custom or wavefront LASIK vision correction procedures. But some eye doctors use this advanced technology into their routine eye exams as well.

Slit lamp exam
A slit lamp is a binocular microscope (biomicroscope) that your eye doctor uses to examine your eye under high magnification.
During the slit lamp exam, you will be asked to place your forehead and chin securely against the rests on the front of the instrument and your doctor will begin by examining the structures of the front of your eyes — including your eyelids, cornea, conjunctiva, iris, and lens.
With the help of a hand-held lens, your doctor may also use the slit lamp to examine structures located farther back in the eye, such as the retina and optic nerve.
A wide range of eye conditions and diseases can be detected with the slit lamp exam, including cataracts, macular degeneration, corneal ulcer and diabetic retinopathy, etc.
Glaucoma tests
Testing for glaucoma typically begins with measuring the pressure inside your eyes.
A common glaucoma screening test is non-contact tonometry (NCT). In this test, an instrument emits a brief puff of air at the surface of your eye to indirectly measure the pressure inside your eye (intraocular pressure, or IOP).
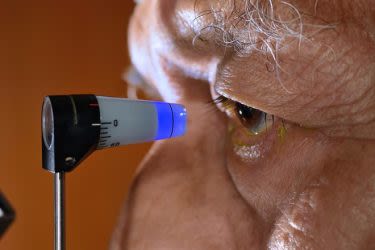
If you have high eye pressure, you may have a high risk of glaucoma.
Another type of IOP monitoring test is called applanation tonometry. The measuring device (which is considered even more accurate than a non-contact tonometer) is a small device that is attached to a slit lamp.
For this test, your eye doctor will put numbing eye drops in your eye that contain a yellow dye. Your eyes will feel slightly heavy when the drops start working. Your doctor will then have you stare straight ahead into a blue light emitted by the slit lamp while he or she gently touches the surface of your eye with the small tonometer probe to measure your IOP.
Like NCT, applanation tonometry is painless. At most, you may feel the tonometer probe tickle your eyelashes. The measurement takes just a few seconds.
You typically have no warning signs of glaucoma until you already have significant vision loss. For this reason, routine eye exams that include tonometry are essential to rule out early signs of glaucoma and protect your eyesight.
Pupil dilation
To obtain a better view of the eye’s internal structures, your eye doctor may apply dilating drops to the surface of your eyes to enlarge your pupils. Full pupil dilation usually take about 20 to 30 minutes.
After your pupils are dilated, you will be sensitive to light because much more light enters your eye. Also, you may notice difficulty focusing on objects up close. These effects can last up to a few hours, depending on the strength of the dilating drops.
Once the drops have taken effect, your eye doctor will use one or more instruments to examine the interior of your eye to rule out health problems such as cataracts, glaucoma, macular degeneration, retinal detachments or other problems of the retina or optic nerve.
Bring sunglasses with you to your eye exam, to minimize glare and light sensitivity on the way home.
Visual field test
In some cases, your eye doctor may want to check for the possible presence of blind spots or restrictions of your peripheral or “side” vision by performing a visual field test. These types of blind spots can indicate eye diseases such as glaucoma or brain damage caused by a stroke or tumor.
Head Doctor
-
Dr Sumi R Jayaswal
Dr Sumi R Jayaswal
11 years experience
Senior Ophthalmologist / Eye Surgeon, and Infection & Immunologist.
View more →
